One of the trickiest problems currently confronting doctors and biomedical scientists is the emergence of treatment resistant diseases. A group of prominent microbiologists recently called for “urgent action” to address the “global crisis” of antibiotic resistance.1
The existence of bacteria that do not respond to antibiotics and cancer cells that survive chemotherapy undercuts our faith that modern medicine can cure what ails us.(a) In order for scientists to tackle such challenges, they must first understand why some disease agents become resistant to therapies that should eliminate them. New knowledge on these issues may lay the path for scientists to develop more effective treatments.
Treatment resistance can develop through many different pathways. The infamous Methicillin-resistant Staphylococcus aureus (MRSA*) acquires a gene that blocks the activity of the most commonly used, most effective antibiotics.(b) In diseases such as cancer or HIV, for which we have effective targeted therapeutics, resistance often emerges via mutation of the targeted genes and proteins. All of these examples of resistance result from heritable genetic changes that spread through populations of disease agents by the forces of natural selection.
While heritable genetic changes seem to be the primary way in which diseases become truly treatment resistant, scientists have discovered that many disease agents may also develop a drug tolerant state. A drug-tolerant bacterium or cancer cell will not be killed by drug treatment, but it also will not be able to proliferate and cause disease like its drug-resistant counterpart. Surprisingly, it seems that tolerance does not necessarily require any genetic mutations and may be an intrinsic component of some diseases.
In cancer, this tolerance comes from a small population of tumor cells known as cancer stem cells.2 These cells possess the same genetic code as the rest of the tumor, but have different growth characteristics and are less sensitive to many anti-cancer drugs. Even when a drug kills most of a cancer, these rare cells are left behind. If they acquire mutations that make them drug-resistant, they can go on to regrow the tumor. This means that an effective treatment must be able to target the common cells that make up the bulk of a tumor as well as the rare cells that lurk in the background waiting to regrow it.
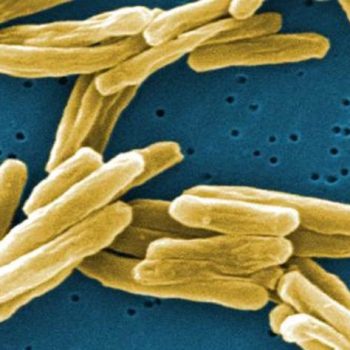
 al, these two populations show different sensitivities to commonly used antibiotics and the slower growing cells tend to be more drug-tolerant. In patients with TB, antibiotic treatment requires upwards of six months, and it has been hypothesized that this lengthy treatment is necessary because of such intrinsic drug tolerance.(c)
al, these two populations show different sensitivities to commonly used antibiotics and the slower growing cells tend to be more drug-tolerant. In patients with TB, antibiotic treatment requires upwards of six months, and it has been hypothesized that this lengthy treatment is necessary because of such intrinsic drug tolerance.(c)
A key finding of this latest paper is that, although the slower-growing mycobacteria were more tolerant of most of the tested drugs, they were actually more sensitive to one antibiotic. This means that the proper combination of antibiotics could target both the fast- and slow-growing populations of cells. A treatment regimen employing these combinations should eradicate the bacteria more quickly, decreasing the risk of mutation and true drug resistance.
Doctors and public health officials emphasize proper and complete use of prescribed antibiotics because exposing an infection to a drug without destroying all of the bacteria can lead to resistance. In the cases of tuberculosis and cancer, intrinsic drug tolerance may result in a similar scenario as a small number of cells survive treatment and create a pool where drug-resistant mutations can develop. By targeting both the intrinsically drug-sensitive and drug-tolerant subpopulations within a bacterial infection or cancer, scientists and clinicians may be able to decrease the likelihood of drug resistance, and increase the efficacy of current and future treatments.
Endnotes
- Karen Bush, et al. (2011) “Tackling antibiotic resistance,” Nature Reviews Microbiology, 9(12): 894-896.
- Craig T. Jordan, Monica L. Guzman, and Mark Noble (2006) “Cancer Stem Cells,” The New England Journal of Medicine, 355: 1253-1261.
- Bree B. Aldridge, Marta Fernandez-Suarez, Danielle Heller, Vijay Ambravaneswaran, Daniel Irimia, Mehmet Toner, and Sarah M. Fortune (2012) “Asymmetry and Aging of Mycobacterial Cells Lead to Variable Growth and Antibiotic Susceptibility,” Science, 335(6064): 100-104.
Sidenotes
- (a) Treatment resistant diseases are also costly. Recent estimates suggest that, each year in the U.S., antibiotic-resistant infections result in $20 billion in health care costs and 8 million extra days in the hospital for patients.
- (b) Antibiotic-resistant MRSA infections are a major concern for doctors and their patients. The CDC estimates there were 94,000 MRSA infections and 19,000 associated deaths in 2005, more deaths than were caused by HIV/AIDS. Although more recent data suggest that MRSA infections are declining, the disease is still a major concern, particularly for individuals with frequent hospitalizations.
- (c) M. smegmatis, the bacteria used in this study, is closely related to M. tuberculosis but is non-pathogenic. Experimenting with M. tuberculosis is quite risky and requires a great deal of specialized equipment and safety precautions. For this reason, M. smegmatis is often used as a safer and easier model for M. tuberculosis.